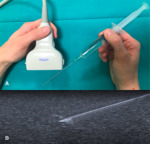
There are two methods to direct the needle relative to the transducer and ultrasound beam: the in-plane approach and the out-of-plane approach.
With the in-plain approach,
the needle is inserted parallel to the transducer and the entire needle shaft and tip is visible at all times during the procedure.
The in-plane approach is the preferred method because continual visualization of the entire needle.
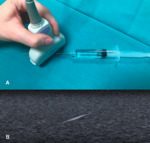
Fig. 1 With the out-of-plain approach,
the needle is inserted perpendicular to the transducer and only a short segment of the needle is seen where the needle passes through the ultrasound beam plane.
Fig. 2 It cannot be determined what segment of the needle is represented on the ultrasound image,
the shaft or tip of the needle,
because they look exactly the same as a single bright echo.
It may be used in more superficial joints (e.g.
small joints of the and foot) [4-7].
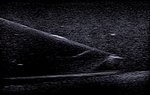
Needle visibility is the best when the needle path is parallel to the transducer,
because under these conditions the ultrasound beam is perpendicular to the needle Fig. 3 [5,
6,
8].
Tips for reducing the insertion angle:
1.
Optimal needle insertion
Start further away from the transducer (>1 cm),
so that you can steepen the insertion angle without hitting the transducer with the needle.
Fig. 4 Insert the needle at a flatter trajectory (<45°),
because the steeper the needle insertion angle,
the more difficult is it to see.
If the joint lies deep or the patient is obese insert the needle at a steeper trajectory or use longer needles [1,
4,
5,
9].
2.
Heel-toeing maneuver
If there is adequate soft tissue,
perform a heel-toe maneuver by pushing the end of the transducer positioned over the deeper part of the needle into the body to bring the transducer face into a parallel arrangement with the needle shaft.
The ultrasound beam will hit perpendicular to the needle shaft,
thus producing optimal visualization.
Fig. 5 It is easier to localize a needle at the beginning of the insertion with a curvilinear (low-frequency) transducer,
because the ultrasound beams are directed perpendicularly at the obliquely oriented needle [5,
6].
3. Oblique standoff maneuver
If the joint is superficial or the needle was inserted under a steep angle place sterile gel under the end of the transducer,
which is next to the insertion site while the other end is anchored on the skin.
Insert the needle either through this gel or just proximal to it.
This allows the transducer to be more parallel to the needle Fig. 6 [5,
6].
4.
Ultrasound beam steering
Modern transducers are capable of altering the angle of the transmitted ultrasound beam mechanically or electronically so that the beam direction is more perpendicular to the needle.
The ultrasound machine combines the echoes from different directions into a single composite frame (compound spatial imaging or multi-beam imaging).
The needle appears as a brightly echogenic line or dot with an acoustic shadow and ring-down artifact farfield on the screen [10].
The needle should not be advanced unless it is seen in its entirety when using the in-plane approach.
Otherwise the procedure is essentially blind and not image guided [6].
Tips for relocating the lost needle or joint:
1.
Transducer manipulation
First look down at the procedure site to ensure that the needle is indeed beneath and parallel to the transducer plane.
Move the transducer side-to-side only 1 mm at a time.
Moving the probe too fast or abruptly is a common reason why the needle is not visualized.
Once you locate only a part of the needle shaft slowly rotate the transducer clockwise or counterclockwise to align the long axis of the transducer with the long axis of the needle.
Fig. 7 During this maneuver,
the needle shaft will progressively “stretch” across the screen if the direction of rotation is correct.
If the needle shaft “shrinks” on the screen,
the direction of rotation is incorrect [6,11].
2.
Needle path correction
The needle and transducer should never be moved at the same time.
If only the needle is seen,
rotate the transducer until you find the joint.
By looking down at the new transducer direction,
adjust the needle into the same plane.
Needle path correction is possible only when the needle is in the subcutaneous fat.
Once the needle enters the muscle tissue and fascial planes,
needle movement is limited and painful [6,
11].
3.
Needle jiggling
Move the needle gently back-and-forth without advancing it.
Look for soft tissue movements adjacent to the needle.
If you cannot visualize the needle itself,
but you see the soft tissue movements,
move the transducer minimally side-to-side and you will most likely relocate the needle in the vicinity of the soft tissue movements Fig. 8 [5-7].
4.
Needle rotation
The orientation of the needle bevel has an impact on the ultrasound image of the needle tip.
Visibility is best with the bevel either directly facing or averting the transducer.
Rotate the needle and you will see the needle tips echo changing due to different bevel orientation Fig. 9 [5,
8,
10].
5.
Injection of anesthetic or sterile saline
To confirm the location of the needle tip inject some anesthetic or sterile saline and look for the spread of hypoechogenic fluid.
When injected into soft tissue or fat pad,
it will ball up Fig. 12 .
Fluid in a perineural or peritendinous location may form a “doughnut sign”.
When injected into the joint,
the joint capsule will distend [2,
5,
7].
6.
Color Doppler and Power Doppler
When injecting anesthetic or saline in order to relocate the needle tip turn on Color Doppler Fig. 13 or Power Doppler Fig. 11 to see a flash.
Avoid puncturing blood vessels by identifying them beforehand with Color or Power Doppler [2,
3,
5].
7.
Air bubbles in the anesthetic or saline
Shake up the anesthetic or saline beforehand to induce air bubbles,
which can act as a contrast medium [12].
8.
Injection of air
Inject a small amount of air.
If injected into the soft tissues it will push the soft tissues apart and disappear,
it will not ball up like the anesthetic or saline.
If injected into the joint capsule,
small bubbles of air will appear in the joint fluid Fig. 10 [12].
9.
Echogenic needles
Echogenic needles have special coated or etched surfaces,
especially near the needle tip,
which reflects ultrasound beams more than plain conventional needles.
The latter may not generate a recordable echo because its rounded shaft reflects most incident sound away from the source Fig. 14 [5-8].
10.
Scratched needles
Make scratches on the needle to make that part of the needle reflect sound beam more.
Use these needles to practice on gel pads,
but never on patients,
because the metal particles from the starched part of the needle can stay in the patient Fig. 15 [6].